The Latest on GLP-1's
Author: Kamryn Hilton, RDN, LDN
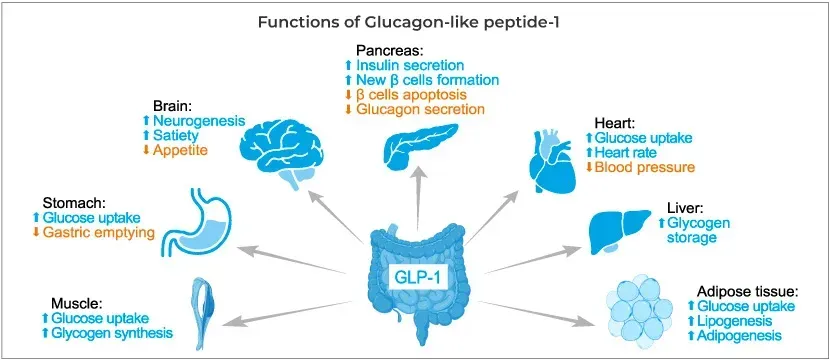
Image: GenScript
The Latest on GLP-1's
GLP-1 receptor agonists are a hot topic in the weight loss industry. If you have been considering using this medication to help reach your physique goals, it is crucial that you are informed of the most up-to-date research, to help you make the best decision for yourself.
Background on GLP-1’s
Most Recent Research on GLP-1’s
Benefits of GLP-1 Use
Initially developed for blood glucose control and weight management, GLP-1 use has led to favorable metabolic and endocrine outcomes, such as lower A1c levels and weight loss.
Studies have also shown improvements in several other areas of the body including cardiovascular health, kidney function, respiratory health, arthritis, sleep apnea, and possibly liver function. This is most likely attributed to the positive outcomes that follow weight loss.
Risks and Concerns of GLP-1 Use
While there are promising benefits many people have experienced through GLP-1 use, those benefits do not come without risk.
Gastrointestinal Effects
The most prevalent adverse effects associated with GLP-1 use include gastrointestinal symptoms, such as nausea, vomiting, diarrhea, and constipation. These symptoms often occur during the initial treatment phase and affect roughly 50-60% of patients. However, they generally diminish over time, and the occurrence tends to be dose dependent.
The gallbladder plays a role in the digestion and absorption of dietary fats by storing, concentrating, and releasing bile (a digestive fluid produced in the liver). Several randomized control trials have demonstrated a significantly higher prevalence of gallbladder disorders among patients using a GLP-1 compared to placebo. Gallbladder issues that have consistently been observed include uncomplicated gallbladder stones, complicated gallbladder stones, cholecystitis with/without gallbladder stones, and biliary obstruction.
Other concerns have arisen from the use of GLP-1’s, such as intestinal obstructions and acute pancreatitis. However, study results are mixed, revealing the need for more extensive research to determine any associations and causations.
Muscle Loss
A decline in skeletal muscle mass and strength (sarcopenia) is increasingly recognized as a significant comorbidity in patients with type 2 diabetes and obesity. Clinical trials consistently show that GLP-1 therapy results in small but measurable decreases in lean mass. This is most likely attributed to lack of physical activity (especially resistance training) and inadequate protein intake. Preserving skeletal muscle is critical for metabolic health, physical function and long-term outcomes. In fact, losing muscle actually slows down your metabolism, making it harder to lose weight and easier to regain weight in the long run. While further research is needed to determine nutrition and exercise strategies to prevent muscle loss, it is recommended that most people on GLP-1’s aim for 1.2–1.6 g/kg adjusted body weight of protein daily, and engage in regular strength training. Unfortunately, one study revealed that less than half of those on a GLP-1 actually achieve the minimum protein recommendations each day, and many report not having the energy to strength train considering their hypocaloric state.
Nutrition Deficiencies
As their use increases, more evidence suggests that these medications may predispose patients to vitamin and mineral deficiencies, especially vitamin D, iron and B-complex vitamins. These gaps in nutrition are often due to a suppressed appetite, reduced food intake, and altered absorption. An observational study done in 2025 noted that over 20% of patients using a GLP-1 developed at least one nutrition deficiency within the first year of use. Deficiencies may also be caused by common gastrointestinal side effects, such as nausea. Considering this growing body of evidence, it is vital that GLP-1 patients adhere to a high protein, nutrient dense diet to achieve optimal health and weight loss.
Other Concerns
There is some concern about GLP-1 receptor antagonists leading to a reduction in bone mineral density due to rapid weight loss, especially in those who do not engage in regular strength training. A very large cohort study recently published by Oxford University concluded that GLP-1 use was associated with a modestly increased risk of fragility fractures in older adults with type 2 diabetes.
Studies have also shown a potential, but low risk of developing pancreatitis. Historically, the FDA has issued warnings of pancreatic cancer with the use of GLP-1's. However, larger studies have come out and have found no significant association. More studies and clinical trials are needed to determine the risk of pancreatitis with the use of GLP-1's and the exact mechanism.
Other Considerations for GLP-1 Users
Duration of GLP-1 Use
Weight regain is common following the discontinuation of GLP-1 therapy.
A recent
systematic review
shows that after one year of treatment cessation, patients regain 60% of the weight they lost during GLP-1 treatment. This presents questions regarding the long-term efficacy of GLP-1 use. More evidence is needed to determine risks and recommendations of long-term use.
Nutrition and Physical Activity Recommendations for GLP-1 Users
Successful GLP-1 use does not come without permanent lifestyle changes. That is why it is crucial for providers to educate their patients on the nutrition priorities while on a GLP-1, especially around the topics of maintaining muscle, preventing nutrition deficiencies, and avoiding future regain. However, there is growing concern for the lack of formal medical training in nutrition and obesity and the lack of competency to provide nutrition counseling. Based on existing guidelines and evidence, many individuals prescribed a GLP-1 are offered general obesity counseling, rather than drug-specific recommendations.
It is absolutely necessary for those receiving GLP-1 therapy to commit to a structured strength training routine, to preserve skeletal muscle and bone mineral density. The current physical activity recommendations in people with obesity on GLP-1's include 60-90 minutes/week of resistance training (broken up in 2-3, 20-30 minute sessions).
GLP-1 Alternatives
Like a GLP-1, high fiber and high protein diets also help regulate blood sugar and appetite. This is because it takes both of these nutrients longer to digest, providing more of satiating effect, while also nourishing your body and providing you sustainable energy. Prioritizing fiber-rich foods such as fruits, vegetables, lentils, beans, and whole grains, and lean proteins like fish, chicken, and lean beef is a great, natural way to help control your hunger and cravings.
There are even certain plants and herbs that may contain similar benefits to a GLP-1. Berberine, for example, is a yellow compound extracted from certain plants that has been used in traditional Chinese and Ayurvedic medicine.
Berberine has been shown to be effective in many studies for blood glucose control and weight management due to its ability to improve insulin sensitivity and regulate the gut microbiota. While this is certainly no magic answer to weight loss, supplementing with this compound, along with following a proper nutrition and exercise protocol, may help you reach your weight loss goals.
Final Thoughts
While countless individuals have experienced a significant amount of weight loss through GLP-1 therapy, it is important to consider all aspects of your health, including long-term effects. Whether you are using a GLP-1 or not, anyone can benefit from following a balanced, nutritious diet and a consistent exercise program, both tailored to them.
If you are ready to lose weight and change your body composition naturally, and KEEP the results for good, click
here to apply for 1:1 nutrition coaching.
Share This Post!
KZ Nutrition Blog



